Medicaid coverage, opioid use disorder treatment, and medication access during the COVID-19 pandemic Aniket Patil, University of Rochester
Principal Investigator
Aniket Patil, Predoctoral Research Associate, Applied Microeconomics, University of Rochester
Co-Investigators
- Alina Denham, Assistant Professor, Family, Population and Preventative Medicine, Stony Brook University
- Daniel Guth, Postdoctoral Fellow, Department of Public Health and Economics, University of Rochester
- Grace Sventek, Grace Sventek, Predoctoral Research Associate, Department of Public Health and Economics, University of Rochester
- Konstantin Kunze, Konstantin Kunze, Postdoctoral Fellow, Department of Public Health and Economics, University of Rochester Tanzy Love, Associate Professor of Biostatistics, University of Rochester Medical Center Sydney Pargman, Predoctoral Research Assistant, University of Rochester
- Robert Hurley, Director, Pain Outcomes Lab, Wake Forest University
- Meredith Adams, Associate Professor, Anesthesiology, Biomedical Informatics, Pharmacology & Physiology, and Public Health Sciences, Wake Forest University School of Medicine
- Elaine Hill, Professor, Departments of Public Health Sciences and Economics, University of Rochester
Funded By
Social, Behavioral, and Economic COVID Coordinating Center (SBE CCC)
The Problem
Medicaid covers half of nonelderly adults with opioid use disorder (OUD). High churn rates disrupt care, impede treatment initiation, and reduce retention. Continuous coverage is vital for medications for OUD (MOUD). The COVID-19 Public Health Emergency mandated continuous enrollment, offering an opportunity to assess its protective effect on the OUD Population.
The Approach
The researchers used Transformed Medicaid Statistical Information System (T-MSIS) data from all states to compare continuous coverage before (2018–2019) and during (2020–2022) the mandate.
They then looked at retention in individuals who were prescribed Buprenorphine, Naltrexone, and Methadone, after acute events such as inpatient stays or emergency department visits. The team also assessed disenrollment among enrollees with ongoing MOUD, stratifying by state, demographics, rural/urban status, and eligibility categories.
The Findings
The researchers found that the 12-month continuous coverage rate for OUD enrollees rose from 78.2% in 2018–2019 to 95.1% in 2020–2022.
Continuous enrollment policies substantially reduce Medicaid churn in this vulnerable population, safeguarding MOUD recipients from losing coverage, improving treatment retention, and sustaining recovery.
As Medicaid extends continuous coverage to young children and postpartum women, policymakers could consider a similar approach for the OUD population to help more effectively combat the opioid crisis, reducing overdoses.
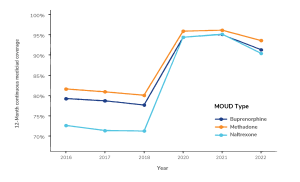
Line graph illustrating “12-month Continuous Medicaid Coverage” rates for three MOUD (medication for opioid use disorder) types: Buprenorphine (blue), Methadone (red), and Naltrexone (green), from 2016 to 2022. Coverage rates are on the y-axis (from 70% to 100%), and years are on the x-axis. All three MOUD types show stable coverage rates from 2016 to 2018 (Buprenorphine: ~79%, Methadone: ~81%, Naltrexone: ~72%) and a sharp increase between 2018 and 2020. Methadone reaches 95% in 2020 and 2021, before slightly declining in 2022. Buprenorphine and Naltrexone peaks just above 94% in 2020 and 2021, then drops to ~91% in 2022. A legend identifies the three MOUD types with their corresponding color lines and markers.