State policy contexts, COVID-19 response policies, and mental health among U.S. working-age adults
Principal Investigator

Shannon M. Monnat
Lerner Chair in Public Health Promotion and Population Health, Director of the Center for Policy Research, and Professor, Department of Sociology, Syracuse University
Co-Investigators
- Iliya Gutin, Research Assistant Professor and Senior Research Associate, Lerner Center for Public Health Promotion and Population Health and Center for Aging and Policy Studies, Syracuse University
- Jennifer Karas Montez, University Professor, Sociology Department, Syracuse University
- Emily Wiemers, Associate Professor, Public Administration and International Affairs Department, Syracuse University
- Douglas A. Wolf, Professor Emeritus, Public Administration and International Affairs Department, Syracuse University
Funded By
The problem:
Many studies in recent years have documented a sizable decline in mental health in the United States that predates the COVID-19 pandemic. There are many reasons to believe this trend continued through, and was likely exacerbated by, the pandemic; however, more research is needed to better understand the contextual determinants of poor mental health in the United States. This is particularly true as national trends tend to obscure considerable subnational variation–especially when it comes to states’ roles in shaping numerous health-relevant policies
Despite the importance of states as structural determinants of health, it is largely unknown whether the decline in mental health in the US varied across the country, and in turn, how individual state policy contexts may or may not exacerbate this trend. As such, there is little knowledge of the potential mental health consequences of exposures to different state policy contexts, even while there is a robust and growing body of research on the effects of state policy contexts for physical health and mortality. The researchers aim to fill a gap in knowledge regarding whether variation in mental health across US states is associated with the kinds of policies states adopt.
The approach:
The researchers aimed to examine how adult mental health over a 30-year period was associated with major changes in states’ policy contexts during that period, combined with states’ policy responses to the COVID-19 pandemic starting in 2020. To understand the significance and magnitude of this relationship, the researchers integrated the following state- and individual-level data:
Behavioral Risk Factor Surveillance System (BRFSS) 1993–2022: Individual-level survey data on such factors as the number of poor mental health days in a month.
BRFFS data allow for a closer look at some of the individual-level covariates that are likely to impact mental health outcomes such as race, age, and sex.
State Policy Conservatism: Places states on a spectrum from liberalism to conservatism such that researchers could gain a general sense of a state’s policy environment.
There are many policies, across policy domains that are likely to matter by both their direct and indirect effects on mental health.
Oxford COVID-19 Government Response Tracker: Collects fine-grain, state-level COVID policy data between 2020–2022.
The researchers focused on two aspects of the tracker’s data:
- Monthly Stringency Index, which measures the strictness of physical distancing policies.
- Monthly Economic Support Index, which measures the generosity of income support and debt relief.
The findings:
As state policy contexts become more conservative across a broad range of policy domains, the researchers observed worse mental health among residents. This held true regardless of operationalization (i.e. number of poor mental health days or a measure of extreme distress).
This finding reaffirms the focus on state policy context as a fundamental determinant of population health, especially when it comes to the many mechanisms by which these policies operate and how they are reflected across a broad range of health outcomes.
More work is needed to try and isolate the effects of state policy contexts from the myriad other state-level factors that are at play. In upcoming work, this team seeks to understand who may be driving these associations, that is, understanding in which subpopulations these associations are having the strongest impact.
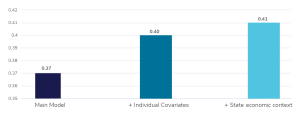
Bar chart titled “Change in probability of ‘extreme distress’ with increasing state policy conservatism.” Three vertical bars illustrate changes in probability for different model adjustments, with probability values marked in light gray above each bar.
From left to right:
The first bar (dark blue, labeled “Main Model”) shows a probability of 0.37, marked with two asterisks for significance (**).
The second bar (blue with white dots, labeled “+ Individual Covariates”) shows a probability of 0.40, marked with two asterisks (**).
The third bar (blue with white dots, labeled “+ State Economic Context”) shows a probability of 0.41, marked with three asterisks (***).
The y-axis ranges from 0.35 to 0.42. The chart indicates that the probability of “extreme distress” increases with state policy conservatism and with the inclusion of individual and state-level economic covariates.
Selected Publications & Presentations
Monnat, S. M. (2021). Rural-Urban Variation in COVID-19 Experiences and Impacts among U.S. Working-Age Adults. The ANNALS of the American Academy of Political and Social Science, 698(1), 111–136. https://doi.org/10.1177/00027162211069717
Monnat, S. M., Wheeler, D. C., Wiemers, E., Sun, Y., Sun, X., Wolf, D. A., & Karas Montez, J. (2023). U.S. States’ COVID-19 physical distancing policies and working-age adult mental health outcomes. Preventive Medicine Reports, 35, 102370. https://doi.org/10.1016/j.pmedr.2023.102370
Montez, J. K., Monnat, S. M., Wiemers, E. E., Wolf, D. A., & Zhang, X. (2024). Stability and Volatility in the Contextual Predictors of Working-Age Mortality in the United States. Journal of Health and Social Behavior, 00221465241271072. https://doi.org/10.1177/00221465241271072
Sun, Y., & Bisesti, E. M. (2023). Political Economy of the COVID-19 Pandemic: How State Policies Shape County-Level Disparities in COVID-19 Deaths. Socius, 9, 23780231221149904. https://doi.org/10.1177/23780231221149902
Wolf, D. A., Monnat, S. M., Wiemers, E. E., Sun, Y., Zhang, X., Grossman, E. R., & Montez, J. K. (2024). State COVID-19 Policies and Drug Overdose Mortality Among Working-Age Adults in the United States, 2020. American Journal of Public Health, e1–e9. https://doi.org/10.2105/AJPH.2024.307621
Zhang, X., & Monnat, S. M. (2024). Watchful, skeptics, and system distrusters: Characteristics associated with different types of COVID-19 vaccine hesitancy among U.S. working-age adults. Vaccine, S0264410X24007217. https://doi.org/10.1016/j.vaccine.2024.06.047