Increases in cardiac mortality 2020-2024: Deadly aftershocks of the pandemic
Principal Investigator

John Hsu
Director of the Program for Clinical Economics and Policy Analysis, Mongan Institute for Health Policy, Massachusetts General Hospital; Associate Professor of Medicine, Department of Medicine, Harvard Medical School; Associate Professor, Department of Health Care Policy, Harvard Medical School
Co-Investigators
- Jason Wasfy, Associate Professor of Medicine, Harvard Medical School; Mongan Institute, Massachusetts General Hospital
- Yuqian Lin, Analyst, Mongan Institute, Massachusetts General Hospital
- Mary Price, Analyst, Mongan Institute, Massachusetts General Hospital
- Deborah Blacker, Professor, Department of Epidemiology, Harvard School of Public Health; Professor, Department of Psychiatry, Massachusetts General Hospital
- Joseph Newhouse, Professor, Department of Health Care Policy, Harvard Medical School
Funded By
The problem:
Health systems faced multiple shocks, increasing mortality, and shifts in medical care use in 2020. The team looked at cardiac emergencies–which are particularly poised to serve as a sentinel condition– since most serious cases can be captured as they require medical care at some point. In these cases, time is of the essence for care delivery. As a result, cardiac emergencies reveal crucial insights into the health system function and structure, including timing: such as when people show up to seek care, how long they wait, and more.
Yet, in 2020, there were early, predominantly single-facility reports of a decrease in emergency department visits for Acute Myocardial Infarction (AMI) hospitalizations as places were facing outbreaks.
The approach:
In this study, John Hsu and colleagues examined changes in cardiac mortality in Massachusetts from 2020 to 2024, highlighting the lasting health impacts of the COVID-19 pandemic.
Using state death certificate data and predictive modeling, the study finds persistent increases in cardiac deaths beginning in 2020, with notable shifts in where deaths occurred (e.g., home, long-term care facilities, outpatient/EDs, inpatient, other, or unknown). These trends are attributed to both biological (e.g., infection) and non-biological (e.g., care avoidance, system disruptions) pathways. The findings underscore how pandemic-related shocks have had enduring and uneven effects on cardiovascular health.
The findings:
Despite initial reports that AMI rates were dropping substantially in early 2020, the researchers could not find a plausible explanation for the magnitude of this change. After further analysis, they actually found persistent increases in cardiac mortality over several years and increases in population-level deaths starting in 2020. Further, these deaths reflect shifts in location (there were more deaths at home than in medical facilities) and display exaggerated seasonal patterns.
These findings raise a host of questions around biological pathways (disease burden around respiratory illnesses) and nonbiological pathway concerns (delaying care, workforce shortages, backlogs and crowding in EDs, shifts in care, and more). Further research is needed to understand the series of shocks precipitated by the pandemic and the resulting shifts in how people sought and used care.
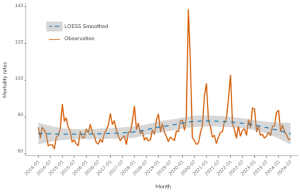
Line graph titled “All-cause mortality rates (per 100,000 MA population)” showing monthly mortality rates from January 2014 to July 2024. The y-axis displays mortality rates ranging from 60 to 140. The orange line represents observed mortality rates, which fluctuate over time with noticeable peaks, especially a large spike around early 2020. The blue dashed line shows LOESS smoothed mortality rates with a gray shaded confidence band. The legend indicates blue for “LOESS Smoothed” and orange for “Observed.” Mortality rates also spike in early 2021, early 2022, then decline towards mid-2024.
Selected Publications & Presentations
Hsu, J., Chin, C. Y., Weiss, M., Cohen, M., Sastry, J., Katz-Christy, N., Bertko, J., & Newhouse, J. P. (2021). Growth In ACA-Compliant Marketplace Enrollment And Spending Risk Changes During The COVID-19 Pandemic. Health Affairs, 40(11), 1722–1730. https://doi.org/10.1377/hlthaff.2021.00501
Festa, N., Katz‐Christy, N., Weiss, M., Lisk, R., Normand, S., Grabowski, D. C., Newhouse, J. P., & Hsu, J. (2023). Nursing home infection control strategies during the COVID‐19 pandemic. Journal of the American Geriatrics Society, jgs.18402. https://doi.org/10.1111/jgs.18402
Weiss, M., Normand, S.-L. T., Grabowski, D. C., Blacker, D., Newhouse, J. P., & Hsu, J. (2024). All-cause nursing home mortality rates have remained above pre-pandemic levels after accounting for decline in occupancy. Health Affairs Scholar, 2(11), qxae126. https://doi.org/10.1093/haschl/qxae126