Disparities in pregnancy-related outcomes during the COVID-19 pandemic
Principal Investigator

Elaine Hill, Departments of Public Health Sciences and Economics, University of Rochester
The problem:
Adverse maternal health outcomes have increased over time, and the COVID-19 Pandemic only worsened this crisis. In this study, researchers aimed to (1) examine the quality of Medicaid claims data for pregnancy-related outcomes and (2) understand how the Pandemic affected disparities in adverse outcomes for pregnant and postpartum women.
The approach:
Using national Medicaid enrollment and claims data, the researchers identified a cohort of individuals who were ever pregnant in each year from 2017-2021 and defined specific pregnancy outcomes (i.e., live births, miscarriages, stillbirths, and abortions).
The researchers then compared the live birth numbers in Medicaid claims to births paid for by Medicaid from the National Vital Statistics System (NVSS) to provide evidence on the quality of the Medicaid claims by state. Time trends for mortality during pregnancy, in early postpartum (within 42 days of birth), and in late postpartum (42 to 365 days after birth) were also tracked.
The findings:
In total, the research team identified 8,187,880 individuals with a live birth between January 2017-December 2021.
The rate of early postpartum mortality increased from 8.9 per 100,000 live births before the Pandemic (January 2017-February 2019) to 13.0 per 100,000 live births after the start of the Pandemic (March 2020-December 2021). Over that same time period, the rate of late postpartum mortality increased from 28.0 per 100,000 live births to 38.3 per 100,000 live births.
These unadjusted rates do not account for increases in Medicaid enrollment length following the declaration of the Public Health Emergency.
Within these data, the researchers found compelling evidence of increased racial disparities over this time period. From before the Pandemic to after the start of the Pandemic, the rate of early postpartum mortality among non-Hispanic White mothers, non-Hispanic Black, and Hispanic mothers increased by 15.7%, 57.8%, and 48.4%, respectively. For late postpartum mortality, non- Hispanic White mortality increased 21.3%, non-Hispanic Black mortality increased 74.3%, and Hispanic mortality increased 41.6%.
These findings indicate that while there are some data concerns, Medicaid claims can be used to study outcomes for pregnant and postpartum individuals. Moreover, the worsened postpartum outcomes following the COVID-19 Pandemic, highlight the continued need for policy interventions targeted at improving postpartum health, and more specifically, at reducing disparities.
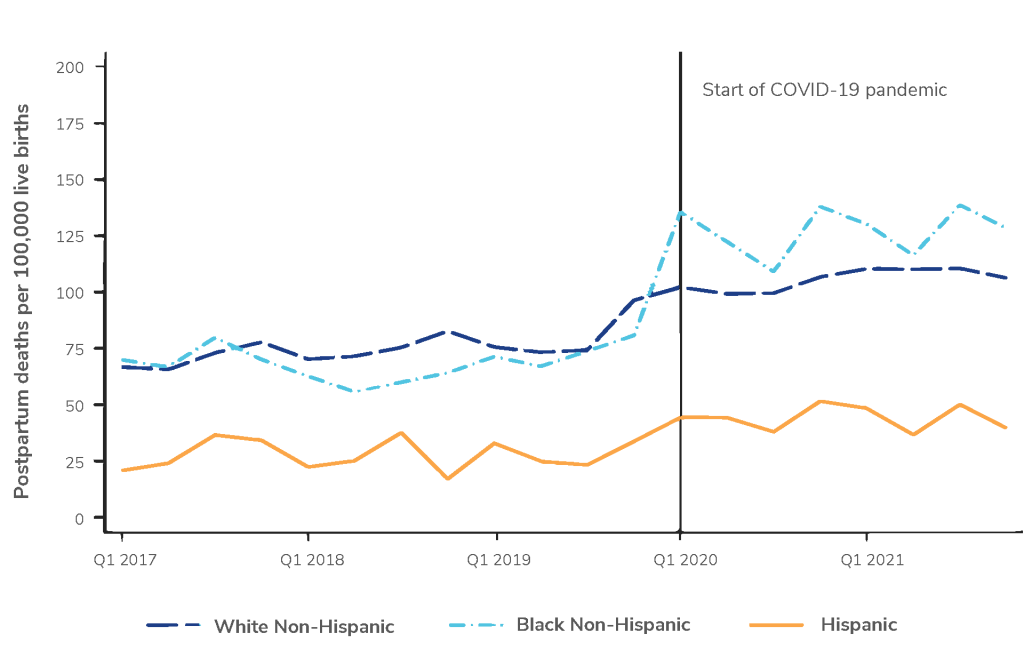
Line graph showing postpartum deaths per 100,000 live births by race/ethnicity (White Non-Hispanic, Black Non-Hispanic, and Hispanic) from Q1 2017 to Q1 2021. A vertical line marks the start of the COVID-19 pandemic at Q1 2020. Before the pandemic, postpartum deaths for Black Non-Hispanic and White Non-Hispanic groups were relatively stable, while Hispanic rates were lower and showed less fluctuation. After the COVID-19 pandemic began, postpartum death rates increased for all groups, with Black Non-Hispanic individuals consistently having the highest rates, followed by White Non-Hispanic, and then Hispanic individuals, who had the lowest rates.